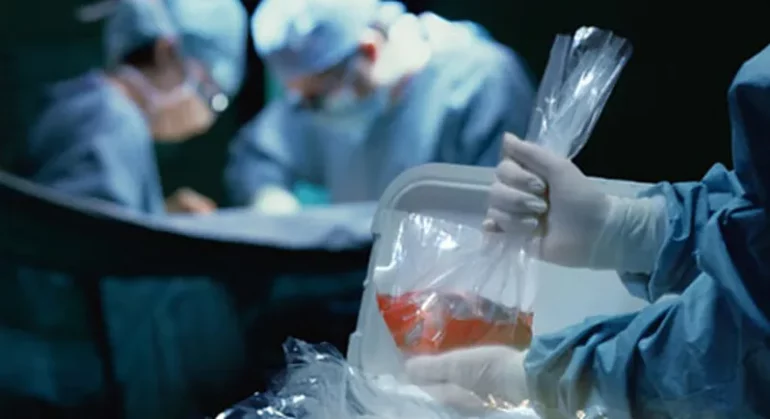
The illegal harvesting of one of the kidneys of a middle-aged woman, Kehinde Kamal, in a private hospital in Nasarawa State and the removal of a portion of the intestine of a 13-year old patient, Adebola Akin-Bright at a hospital in Lagos during surgical operation are a bad omen for the country, indicating increased need to protect patients.
Forced organ harvesting is the practice of surgically removing a victim’s organs against his or her will. They are then sold on the black market for transplantation in the body of other people. It was learnt that about 10 per cent of the world’s population suffers from chronic kidney disease. Between two and seven million of these patients are estimated to die every year because they lack access to proper treatment. Under these circumstances, desperate patients seek illegal ways to obtain organs outside their home countries, and some unethical doctors are available to steal and sell the vital part of the body.
Because life is what is being tinkered with when surgical tasks are being performed, especially complex ones around the vital organs of the body, the procedure should be properly managed so that the patient does not fall a victim of negligence and illegal organ harvesting by any doctor. Organ harvesting is illegal in Nigeria under the Trafficking in Persons Prohibition, Enforcement and Administrative Act with a punishment of seven years jail term or a fine of N5million.
The rising cases of poorly managed surgical procedures in some hospitals leading to unexplainable disappearance of vital organs in the body is fuelling serious distrust in the quality of local healthcare and preference for medical care abroad that has cost the nation billions of naira.
More worrisome is the belief now that some surgeries are deliberately recommended with the hidden intent to steal vital organs of the unsuspecting patients, thereby ruining their lives, some resulting in death. There is, therefore, a need to initiate stronger protection for patients such that they can get a clear and complete receipt of their organs through medical tests before and after a surgical procedure.
A medical doctor, Noah Kekere, in Jos North Local Government Area of Plateau State was recently arrested by the police for allegedly removing one of the kidneys of Kehinde Kamal while attending to her in his clinic. Husband of the patient, Alhaji Kamal alleged that when his wife complained of abdominal pain in 2018, he contacted the doctor who diagnosed her of appendicitis that needed to be removed through operation.
“We paid for the full cost of the drugs and the hospital bill as directed by the doctor. My wife was sound before the operation but shortly after the operation, she started complaining of severe pain. We managed the pain for years while visiting the same doctor. Around August ending, the pain got extreme and we had to go to the Jos University Teaching Hospital where it was confirmed that my wife had her kidney removed,” Kamal recounted.
The case of Akin-Bright has pitted the private hospital and the government hospital that attended to him against each other as regards who to blame for the poor surgical procedure that led to the cutting of his intestine. It was learnt that a medical doctor, Abayomi Baiyewu, who is not a certified surgeon, performed two surgeries on Akin-Bright at Obitoks Hospital, a private healthcare centre in Alimosho Local Government Area of Lagos. At the request of the parents eight days after the operation, the boy was referred to the Lagos State University Teaching Hospital (LASUTH) where another corrective surgery was initiated at the point of obstruction of the patient’s intestine during which 4 inches out of the 24 feet of the normal small intestine were removed. The operation was performed during the 28-day admission of the patient at LASUTH and during which the mother of the boy cried out that her son’s intestine had ‘disappeared’. A panel set up by the Health Facility Monitoring and Accreditation Agency (HEFAMAA) confirmed that the x-ray tests done while Akin-Bright was on admission at LASUTH also showed the presence of the intestine.
Among the reasons people patronise hospitals is the belief that the medical professionals who work in the health institutions were well trained and are ethically sound to deliver high quality healthcare that guarantees safety of life of patients. People feel safer in the hands of trained medical doctors and other health professionals, which is the reason they always submit themselves to be treated for their ailments as recommended by the experts. A patient does not expect to suffer any other threat to his life whenever being attended to by qualified doctors. It is not too different from the practice of entrusting money and other valuables to a bank. It is all about safety, and when the bank actually takes custody of the valuables, the customer feels safe.
Failure of the bank to make these items available when needed by the customer will be a huge disappointment. It is trust that makes patients consent, either by themselves or their relatives, that surgeons should open their h10earts, brains and other highly sensitive parts or organs of their body during complex medical treatments, knowing that any little mistake or negligence in the process could lead to their death or permanent disability. It is the same trust that makes patients swallow drugs recommended by a doctor not knowing whether the drugs can also kill. A hospital is known to be an institution providing medical and surgical treatment and nursing care for sick or injured people.
When people begin to have reason to feel that their lives may no longer be safe in the hands of a medical doctor, when patients become afraid of approaching a doctor or any other health professional for treatment of their diseases, not only the patients but also the society or the environment is in serious trouble. When kidneys begin to disappear during surgical procedures to treat appendicitis, and the problem that makes patients visit hospital is not as serious as the new one they got while being attended to by doctors, then hospitals will begin to attract a new definition.
The government at all levels, professional bodies and human rights groups must be awake to their responsibilities to douse the tension being generated by the organ theft scare in the health sector.
More than ever before, patients in the country need stronger protection. Health experts affirmed that the ethics of the profession do not permit any doctor or any professional to remove any body organ for any non-professional reason. According to a professor of Public Health at the College of Medicine, University of Lagos, Akin Osibogun, by the standard procedure (in the case of Akin-Bright), if there was intestinal obstruction and a portion of the intestine died, it will have to be removed but it must be communicated to the relatives of the patient, and if they like the doctor can give them what he removed. “If they failed to communicate, you can’t also blame the relatives for assuming or suspecting any kind of thing,” he said.
Also, people should raise the alarm and notify relevant agencies such as the HEFAMAA when they notice signs of quackery. There is a need for proper licensing and accreditation of private hospitals to make sure they meet basic standards of quality and safety; they are well equipped with quality surgeons and other experts before being allowed to carry out surgery. A professor of Medicine, College of Medicine, Lagos University Teaching Hospital (LUTH), Olufemi Fasanmade who noted that not all doctors could perform surgery lamented that the practice has not been adequately regulated in Nigeria’s health sector. “If a professor of nursing goes and starts operating, he can be arrested because it is not his field. It’s not his area, especially if the patient dies. Those are the things that regulate our practice,” he said.
Though it may cost more, it is advisable that patients request for a post-surgical scan overviewing their body system to be sure of what has happened to them, especially to be sure that the vital organs are still intact.
On the part of the patients, when the surgery is not urgent, they should carefully assess policies and procedures that are in place in a hospital to ensure the quality and safety of the surgical care. According to the World Health Organisation (WHO), evidence shows that when patients are treated as partners in their care, significant gains are made in safety, patient satisfaction and health outcomes. Patient safety is not a wish but a right that should be guaranteed and promoted.